Correct answer: c.
Discussion
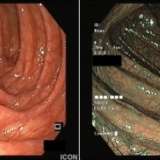
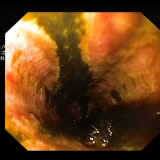
This is a firm nodule covered with a relatively normal-looking mucosa. The differential diagnosis thus rests between a NET and a GIST, both of which arise below the surface mucosa. Endoscopically, the lesion looks more like a NET with its typical dilated vessels close to the head of the polyp. The incidence of NETs is increasing and is now around 5.25/100,000/year.1 Up to 30% of NETs are found in the stomach,2 where they are subclassified into three distinct groups:
- Type 1 NETs are the most common type (they account for 70%–80% of all gastric NETs). Type 1 NETs are associated with achlorhydria (e.g. due to chronic atrophic gastritis or pernicious anaemia), where high levels of gastrin induce hyperplasia of histamine-secreting cells in the gastric body that are called enterochromaffin-like (ECL) cells. The continuous stimulation of the ECL cells to grow ultimately leads to the growth of multiple small carcinoid tumours in the gastric body. In this case, the patient has symptoms of reflux oesophagitis, which eliminates the possibility that the lesion is a type 1 NET. Patients with atrophic gastritis and achlorhydria are unlikely to complain of heartburn!
- Rarely, NETs are associated with pancreatic or duodenal gastrinomas as part of the Zollinger–Ellison syndrome or multiple endocrine neoplasia type 1 (MEN 1). These are called type 2 NETs and they only account for about 5% of cases. Patients with type 2 carcinoids have high gastrin levels and high acid levels and therefore present with symptoms of peptic ulcer disease, diarrhoea or reflux esophagitis.3 Endoscopically, type 2 NETs appear similar to type 1 NETs, with multiple, small gastric nodules. However, there is no gastric atrophy in the surrounding mucosa of type 2 NETs. For this reason, it is important to not only sample the lesion but also the surrounding mucosa in cases of suspected NETs. Type 2 NETs are more aggressive than type 1 NETs—at the time of diagnosis, up to 30% of patients have lymph-node metastases and up to 10% have liver metastases.4
- Finally, sporadic NETs of the stomach (type 3 gastric NETs) are usually single, large (>1 cm in 70%) and aggressive. In more than 70% of cases, there are lymph-node metastases and/or distant metastases at the time of diagnosis.5
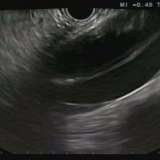
As this is a single, large lesion with dilated vessels leading up to the head of the polyp, the best guess for endoscopic diagnosis is that this is a type 3 NET! To save time, I would now set in motion the standard ‘carcinoid workup’. This workup includes measurement of plasma chromogranin A (pCgA) levels. CgA is produced by all cells derived from the neural crest and high levels are found particularly in patients with metastatic disease. In addition, you should request a ‘gut hormone screen’ (measurement of gastrin, glucagon, vasointestinal peptide, somatostatin and pancreatic polypeptide levels). Finally, you should request either an ‘octreotide scan’ (somatostatin receptor scintigraphy) or, even better, a PET/CT scan using peptides that bind to somatostatin receptors (68Gallium-DOTA-TOC/NOC/TATE).6
What about management of gastric NETs? As type 1 NETs are usually benign, it has been recommended that patients who have up to six nodules that are no larger than 2 cm may be managed endoscopically.7 However, patients with a larger lesion or more than six carcinoids are considered for local surgical resection.8 Of course, an antrectomy would eliminate the source of the hypergastrinaemia and may also result in tumour regression.9
In patients who have type 2 NETs (secondary to an endocrine syndrome), somatostatin analogs may result in regression of the gastric NET.10 However, treatment is also aimed at finding and resecting the primary duodenal or pancreatic tumour that is driving the syndrome.
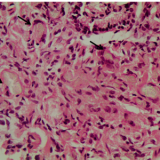
Type 3 NETs are managed in the same way as gastric cancers, with at least a partial gastrectomy and lymph-node dissection. After resection, the mitotic rate within the tumour is assessed by immunohistochemistry. This allows the tumour to be graded according to the WHO classification (grade 1, ≤2%; grade 2, 3–20%; grade 3, >20%).
In this particular case, a subtotal gastrectomy was carried out and revealed a WHO grade 2 sporadic (type 3) NET that was confined to the mucosa and submucosa. However, 2 out of 25 lymph nodes contained metastatic disease!
Please log in with your myUEG account to post comments.