Bjorn Rembacken is at Leeds Teaching Hospitals NHS Trust, Leeds, UK. He was born in Sweden and qualified from Leicester University in 1987. He undertook his postgraduate education in Leicester and in Leeds. His MD was dedicated to inflammatory bowel disease. Dr Rembacken was appointed Consultant Gastroenterologist, Honorary Lecturer at Leeds University and Endoscopy Training Lead in 2005. Follow Bjorn on Twitter @Bjorn_Rembacken
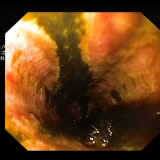
This is a clip from the resection of a duodenal polyp situated at the junction between the duodenal cap and D2.
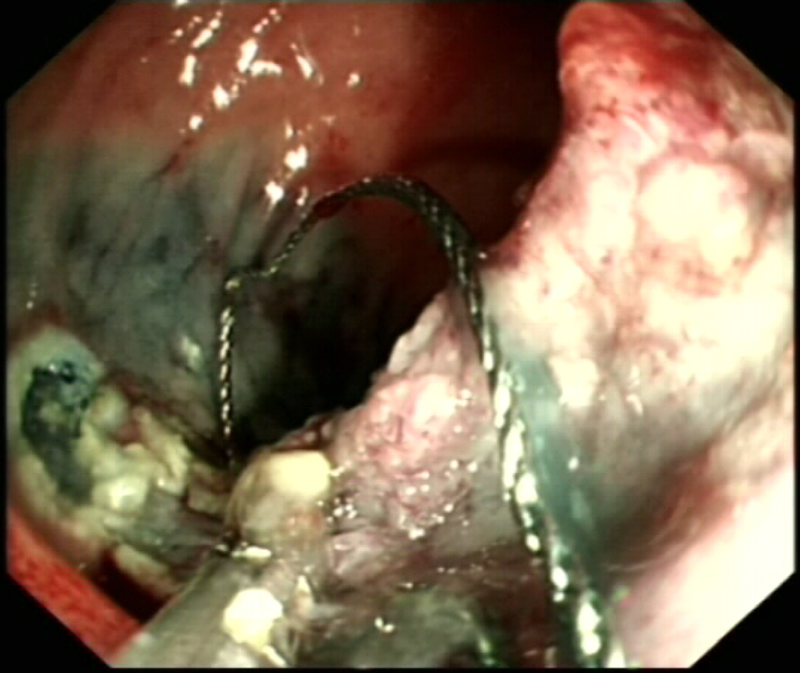
Case Question 1
The procedure was carried out under general anaesthesia and having seen the video clip of the middle and the end of the procedure, how would you advice the patient after he has come around following the anaesthetic?
a)The procedure went very well and you will be able to go home this afternoon
b)The procedure went very well but we will keep you in hospital for observation over night
c)The procedure probably went well but we will keep you “nil by mouth” and keep you in hospital for observation over the weekend
d)The procedure didn’t go according to plan and we will now start intravenous antibiotics and will organise a contrast enhanced CT scan
e)The procedure went very wrong and we are now organising for you to undergo emergency surgery
Discussion
Thanks to everyone for adding to the discussion ! I have the greatest respect for duodenal EMR’s. It is an unforgiving area to work in. The late bleeding rate approaches 10% following larger resections. The vascular supply is rich and the enzyme-rich environment will make sure that any clot which is "doing a job", is promptly digested. Then we have perforations! The muscle propria layer is extremely flimsy and in this case I think that it’s more a thin tear than the usual punched out perforation we see elsewhere in the GI tract. For this reason the “target sign” is unreliable in the duodenum.
If you look at the video clip carefully, you see a small bubble coming out of the tiny perforation close to the clip. I did struggle to close the defect and in the end the patient had to go to surgery. As there was no “contamination”, drains were placed and the area washed out. Nevertheless, the patient spent a month in hospital as the perforation slowly healed.
A recent audit in Leeds, found that risks increase sharply when lesions larger than 2cm in size are resected. A recent series from Australia put the “danger size” at 3cm. The risk of a perforation can approach 1:30 and for this reason you need nerves of steel, a patient who is fully informed of the risks as well as immediate access to supportive and experienced upper GI surgeons. It is my belief, that this is Tiger Country which should only be entered by the most experienced operators working in a tertiary referral centre.
-
About the Author





Please log in with your myUEG account to post comments.