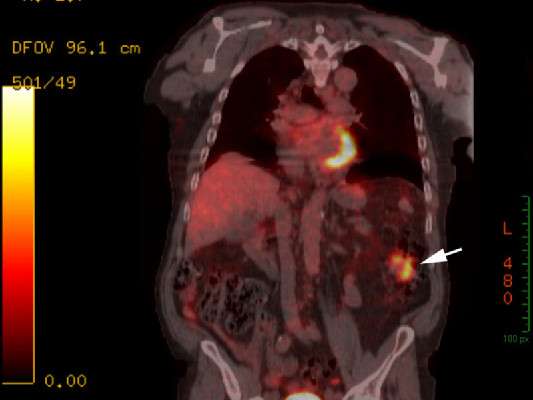
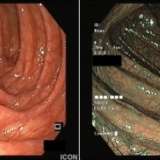
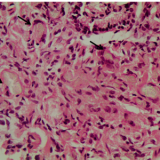
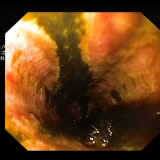
WHAT WOULD YOU DO WITH THESE POLYPS?
a) Ignore them, as they are inflammatory.
b) Take biopsy samples only.
c) Perform standard snare polypectomy.
d) Organise an endoscopic mucosal resection (EMR).
e) Organise an endoscopic submucosal dissection (ESD).

Please log in with your myUEG account to post comments.