Correct answer: A.
Discussion
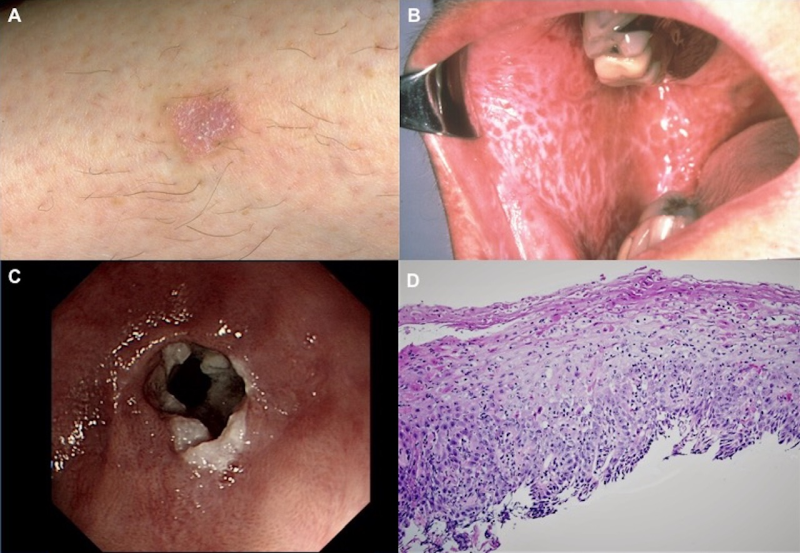
Lichen planus is a condition of unknown aetiology involving the skin, nails and often the mucous membranes. Classically, skin lesions are shiny, violaceous, flat papules (as seen in photograph A) that are mainly found on the front of the wrists, the lumbar region and around the ankles. Mucous membrane lesions complicate 30–70% of cases and consist of white plaques (as shown in photograph B), erosions and, rarely, ulceration inside the mouth or on the tongue, genitalia or anus.
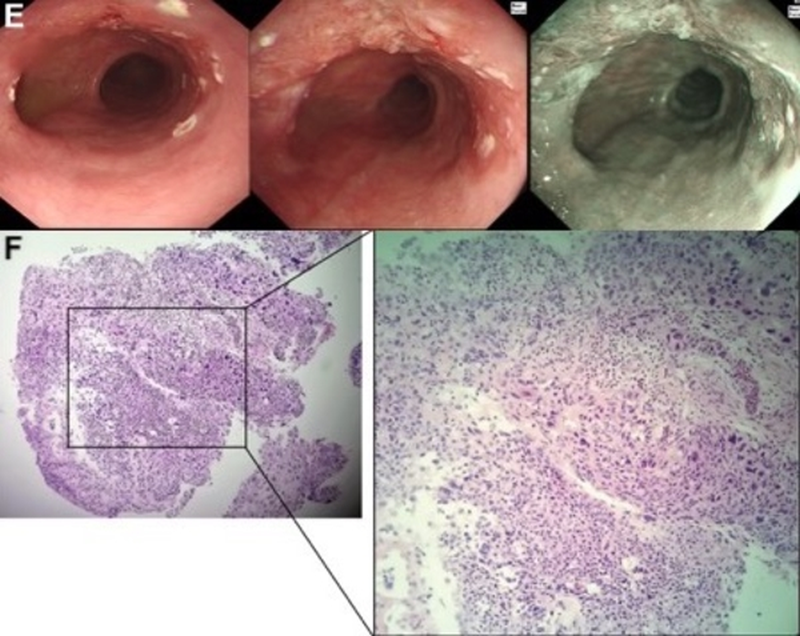
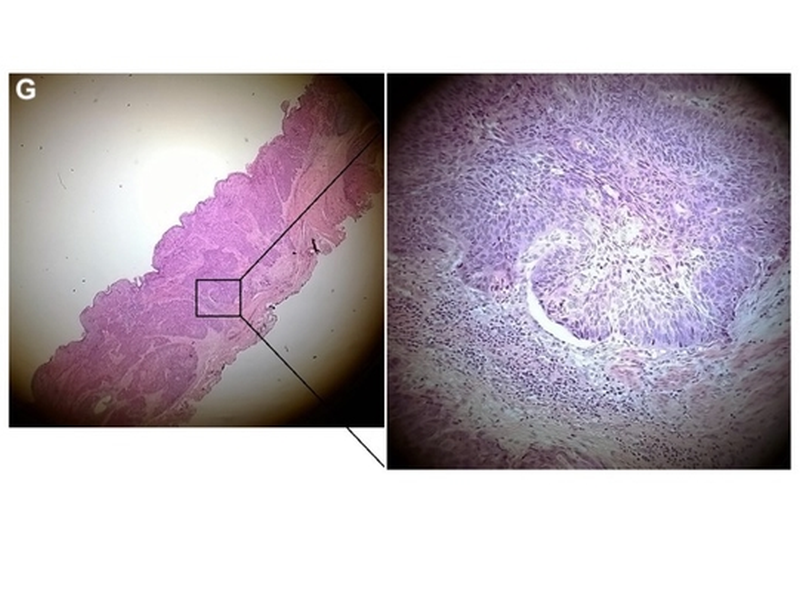
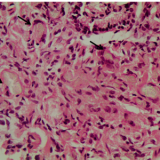
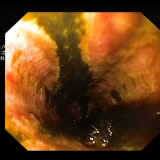
Oesophageal involvement of lichen planus has probably been under-reported.1 Dickens et al.2 reported oesophageal involvement in 5/19 patients and a more recent study by Kern et al. found it in 20/32 patients.3 Oesophageal involvement usually develops in patients who have oral lesions. Indeed, the pathological appearance of lichen planus is similar in the mouth and in the oesophagus, with a band-like lymphocytic infiltrate including ‘Civatte bodies’,4 a nonspecific feature of interface dermatitis that is particularly common on lichen planus. Macroscopically, the oesophageal appearance can include peeling of the friable squamous mucosa, white plaques, ulcers, erosions and strictures,4 and typically affects the proximal oesophagus.
Cutaneous lichen planus is a self-limiting disease, with spontaneous regression of skin lesions within 1 to 2 years; however, both oral and oesophageal lichen planus tend to be chronic. A review from the Mayo clinic reported good results for treatment with topical steroids, fluticasone 880 mcg twice daily or budesonide 3 mg twice daily, with two thirds of patients responding well.5 Of course, any stricturing is managed with dilatations. Dilatations in the absence of medical therapy have been associated with exacerbation of non-oesophageal disease in a Köbner-like phenomenon.6





Please log in with your myUEG account to post comments.