Young GI Blog
The impact on COVID-19 on clinical GI practice – Reports from the front line
May 20, 2020
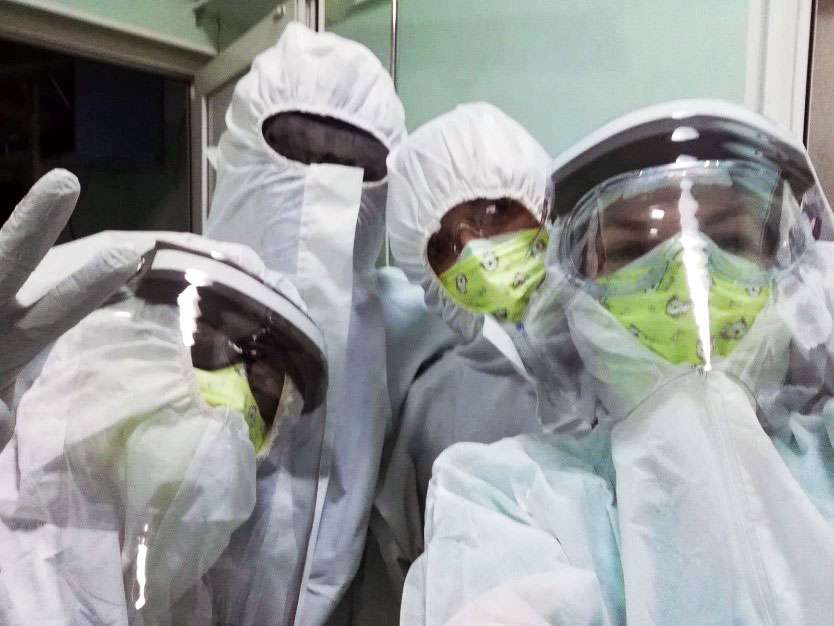
Our colleagues from GI departments across Europe and the Mediterranean have shared some insights as to how the Covid-19 pandemic has changed their clinical practice, as well as their strategies for coping with these new challenges.
We would love to hear about your own experiences, so please comment below with any additional tips!
Iago Rodríguez-Lago, MD PhD
IBD Unit, Gastroenterology Department
Hospital de Galdakao, Galdakao, Spain
This pandemic has hit Spain with an unprecedented impact; both in terms of the number of infected people and sadly, a devastating number of deaths. However, since the first reported cases, workers from all areas of our healthcare system have been doing extraordinary work. After the initial doubts and fears, all the hospital was completely involved in overcoming this crisis. With the aim of avoiding generalized exposure of all physicians to the virus, our Department was divided into three sections: inpatient services, outpatient clinics and endoscopy. Those colleagues who are managing the inpatient services have been caring for patients with COVID-19, and doing a great job under previously unseen pressure. These patients are looked after by a a truly multidisciplinary team, with physicians from the different medical specialties working side by side.
Since the beginning of this emergency, I have been focused on the Inflammatory Bowel Disease outpatient clinic. This is an huge responsibility, as around 1,000 patients are being managed ‘virtually’ for the first time- the arrival of telemedicine! Close daily work with the nursing staff in the clinic and in the infusion day unit has been crucial during the past weeks. Furthermore, thanks to the many tips from different colleagues across the country, we were able to improve many details of our practice. We have learned (again) what we have observed multiple times in the past: teamwork at different levels is the key to success.
We have made multiple changes to our previous practice, and we will see many more during the next months. The endoscopy lists have been completely modified. Medical therapy is now approached with a new ‘benefit-risk’ consideration. Telemonitoring of patients with chronic gastrointestinal diseases will have to be included in our practice going forward. Point-of-care testing for many conditions will become part of daily practice. This situation is a real test to all healthcare providers, but we look forward to a future full of new and interesting advances.
Dr. Vasile Sandru
Gastroenterology and Interventional Endoscopy Clinic
Clinical Emergency Hospital Bucharest, Romania
The first case of COVID-19 in Romania was reported on 26th February 2020, almost one month after the first cases were reported in Italy and Spain. For Romania, the bond with Italy and Spain is very strong; besides sharing a common history and language roots, many Romanians have emigrated to Spain and Italy over the decades. Observing what happened in these countries, and gathering information from our colleagues there, allowed us to try to prepare for what was to come. As time passed, reports from across Europe were becoming progressively more frightening and by 14th March, a National Emergency status was declared in Romania, despite only 97 confirmed cases. We knew that If we were to have a similar case volume in Romania, our Health care system would be overwhelmed quickly.
Hospitals were designated for COVID + patients, with the remaining hospitals carrying on the medical care for all non-COVID patients. Within gastroenterology and endoscopy services, we began to see a decrease in non-urgent outpatient work. We decreased the number of doctors working in the department at any one time, to allow for social distancing, and continuity of care.
Due to issues nationally with the supply of PPE, we decided to use extra plastic protection made of garbage bags, as an extra layer between our normal surgical gowns, mainly for ERCP procedures. We also started to use plastic and plexiglass shields during emergency endoscopy, and bought ourselves face shields, goggles, masks and UVC lamps. We struggled to find FFP2/3 masks as so many retailers had sold out online. There were concerns that the PPE being provided in hospitals was inadequate. However, after 2-3 weeks this improved.
From my personal point of view, I decided to protect my parents who are 60-year-old and 65-year-old respectively and also my 5 months pregnant wife, by staying isolated from them. I have to say that most of my colleagues did the same thing, some being helped to find a place by NGOs or the Government.
As a doctor in a Non-COVID Emergency Hospital, I find it strange because asymptomatic patients may still be carriers, so caution must be observed at all times, no matter what. Starting from one week ago, all the patients admitted in the hospital are tested with rapid tests and PCR. This measure is a great improvement in the safety of patients and medical staff because uncertainty of the status of patients was a significant cause of anxiety.
Our head of Department, Associate Professor Dr. Constantinescu Gabriel has ensured that endoscopy training of our fellows continues, by working in teams, and shifts. We have also started online courses for medical students, as universities have done all over the country.
My thoughts turn to all colleagues who treat patients with COVID in dedicated Hospitals. I would like to assure them of our support and the fact that we do our best to help. In conclusion, a big THANK YOU to all and see you all soon!
Afafe Taiymi
Resident in training - Hepato Gastroenterology unit
Mohammed VI University Hospital Oujda, Morocco
Infection with COVID 19 had a significant impact on my medical GI practice. Several changes were noted:
Impact on hospitalizations:
Our department has been devoted to patients with COVID -19. Therefore, hospitalisation or non-COVID patients has been limited for us, due to a lack of appropriate setting in which to care for them.
All patients with planned hospitalizations were divided into urgent and non-urgent. Only urgent patients have been hospitalised. Most of them have new diagnosis gastrointestinal or biliopancreatic cancers, and require either diagnostic or therapeutic interventions. Non-urgent patients were contacted by phone. The current situation was explained to them, as well as what symptoms were deemed to require urgent care. A telephone number was provided for patients to contact us in emergency situations.
Impact on practice of endoscopy:
A technical platform was arranged with a maximum of equipment needed. For safety, we treated all patients for endoscopy as positive, unless proven otherwise.
All non-urgent endoscopic procedures were postponed according to guidelines. A daily pre-established program is carried out with mobilization of a limited number of medical and paramedical staff. (Two nurses, one or two doctors).
Impact on medical education:
All medical meetings are organized on a virtual platform. We are continuing a regular online course programme 3 times per week. This programme is more intense compared to ordinary days.
Impact on mental health:
Our spirits are up and down, but we do our best to continue spreading the positive vibes and trying to be supportive to each other. We are doing our best to enjoy our work in this ongoing situation and to be in a perfect harmony with all the medical staff.




Please log in with your myUEG account to post comments.